Plantar Fasciitis
- Plantar Fasciitis
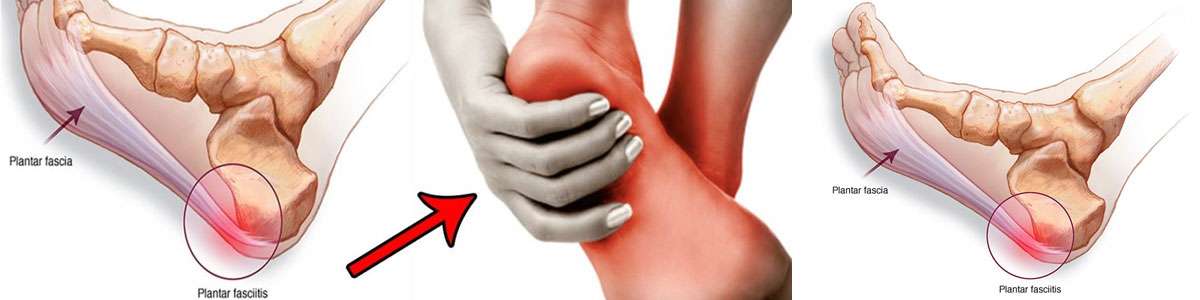
Plantar Fasciitis: Causes, Symptoms, and Treatments
What is Plantar Fasciitis?
Plantar fasciitis is one of the most common sources of heel pain. A plantar fascia refers to a thick fibrous band of connective tissue that originates on the bottom surface of the calcaneus, also called the heel bone and extends along the sole towards the toes. It acts as a passive limitation to the over-flattening of your arch. In situations where the plantar fascia develops micro tears or becomes inflamed, the condition is referred to as plantar fasciitis.
BoynerClinic’s insoles are designed to support the arch, reduce inflammation, and relieve heel pain caused by plantar fasciitis. Book your appointment now with BoynerClinic’s expert care!
What Causes Plantar Fasciitis?
Plantar fasciitis is one of those injuries that seem to occur for no reason. However, plantar fasciitis is caused by two methods, either traction or compression injuries.
The condition can be mostly associated with impact and running sports- especially those that involve toe running rather than heel running styles.
It is also found in people who have poor foot biomechanics that lay stress on the plantar fascia. Therefore, flat feet or weak foot arch control muscles are the two common causes of plantar fasciitis.
1. Traction Plantar Fasciitis
Plantar fasciitis symptoms get aggravated due to traction or stretching forces on your plantar fascia. In other words, your plantar fascia is repeatedly overstretched, leading to plantar fasciitis. The most common reason for the overstretching of the plantar fascia is an elongated arch, which happens due to either poor foot biomechanics or weakness of foot arch muscles.
2. Compression Plantar Fasciitis
Injuries that have a traumatic history can lead to Compression type plantar fascia. For example- landing on a sharp object that causes a bruise on your plantar fascia can be your most likely trauma. You will experience more plantar fasciitis pain under your arch than under your heel, which is presumably a fat pad contusion if a single trauma caused your pain.
The term compression type plantar fasciitis is mostly confused with a fat pad contusion and is often described as a “stone bruise”.
What are the Symptoms of Plantar Fasciitis?
You’ll usually first experience early plantar fasciitis pain under your heel or in your foot arch in the morning when you wake up or after resting. Your heel pain will get worse as you take the first steps but improves with activity as it warms up.
How Does Plantar Fasciitis Progress?
As plantar fasciitis deteriorates, the pain will be present more often. You can determine what stage you are in using the following guidelines:
- No Heel Pain – Normal!
- Heel pain after exercise.
- Heel pain before and after exercise.
- Heel pain before, during and after exercise.
- Heel pain all the time. Including at rest!
The progression of the symptoms stays consistent with the four stages of a typical overuse injury.
Ultimately, if you experience further trauma and delayed healing, it will lead to the formation of calcium (bone) in your plantar fascia. When this takes place next to the heel bone, the condition is called heel spurs, which have a longer rehabilitation period.
At Boyner Clinic, we offer custom-made high arch insoles for plantar fasciitis to help patients get rid of the pain.
How is Plantar Fasciitis Diagnosed?
Plantar fasciitis is either diagnosed by a sports doctor or a physiotherapist. The diagnosis of plantar fasciitis is based on your symptoms, history and clinical examination.
After the plantar fasciitis is confirmed, the doctor will examine why you are likely to be predisposed to plantar fasciitis. Thereafter, they develop a treatment plan to minimise your chances of any future bouts.
The doctor will conduct certain X-rays. If they show calcification in the plantar fascia or at its insertion into the calcaneus, it will be known as calcaneal or heel spur.
Ultrasound scans and MRI are also conducted for determining any plantar fasciitis tears, inflammation or calcification.
You may have to get Pathology tests done, including screening for HLA B27 antigen, to identify spondyloarthritis, which can cause symptoms similar to plantar fasciitis.
Risk Factors for Plantar Fasciitis
You have more chances of developing plantar fasciitis if you are-
Active – If you play sports, that lead to excessive stress on the heel bone and attached tissue. The risk for plantar fasciitis increases, especially when you have tight calf muscles or a stiff ankle due to a previous ankle sprain, which limits ankle movement. For example-. Running, ballet dancing and aerobics.
Overweight – Carrying around extra weight leads to an increase in the strain and stresses on your plantar fascia.
Pregnant – Pregnant women experience weight gain and swelling, which can make their ligaments more relaxed, leading to inflammation and mechanical problems.
On your feet – People with jobs that require them to walk a lot or stand on hard surfaces, such as factory workers, teachers, and waitresses, are more susceptible to plantar fasciitis.
Flat Feet or High Foot Arches – Changes in the foot arch lead to a change in the shock absorption ability. This can stretch and strain the plantar fascia, which then has to absorb the additional force.
Middle-Aged or Older- With ageing, the arch of your foot may begin to sag, putting extra stress on the plantar fascia.
Wearing shoes with poor support.
Weak Foot Arch Muscles – Muscle fatigue makes the plantar fascia overstress and causes injury.
Arthritis- Some types of arthritis can result in tendon inflammation in the bottom of your foot, which may cause plantar fasciitis.
Diabetes – As per research, people with diabetes are at risk of plantar fasciitis. However, doctors have still not been able to determine why plantar fasciitis occurs more often in people with diabetes.
Plantar Fasciitis Treatment
Plantar fasciitis is reversible and can be treated very successfully. As per a study, about 90 per cent of people who have plantar fasciitis see a significant improvement in their condition within two months of initial treatment.
However, if your plantar fasciitis continues even after you receive conservative treatment for a few months, your heel will be injected with steroidal anti-inflammatory medications (corticosteroid). Cortisone injections have some short-term benefits, but they slow down your progress in the medium to long-term. This usually means that you will suffer recurrent bouts for longer.
What is the Best Treatment for Plantar Fasciitis?
As the primary cause of your plantar fasciitis is poor foot biomechanics, it is necessary to conduct a thorough examination and correct your foot & leg biomechanics. This will help prevent any chance of future plantar fasciitis scenarios or the development of a heel spur.
Physiotherapists are highly-skilled and experienced in foot control assessment and dynamic biomechanical correction. As per your specific clinical assessment, the physiotherapist will provide you with certain manual therapy techniques, for example- joint mobilisations to loosen stiff joints, muscle flexibility or stretches, foot taping, foot, soft tissue massage or release, lower limb strengthening exercises and occasionally night splints. The treatment of plantar fasciitis varies from person to person; therefore, it is recommended that you consult with a foot care practitioner for the same.
They may suggest you connect with a podiatrist who is an expert in the prescription of passive foot devices, such as orthotics. There have been numerous cases where foot orthosis has potentially assisted some sufferers of plantar fasciitis.
Your physiotherapist will prescribe some active foot stabilisation exercises that are an excellent long-term solution to prevent and control plantar fasciitis.
Footwear Analysis
The treatment of heel spurs is the same as plantar fasciitis treatment. Your physiotherapist will assess your condition and select the apt treatment modalities for you.
Ultimately, biomechanical correction is the aim. Along with this, foot intrinsic muscle strengthening and calf stretches are required as well.
Cases, where moderate to severe biomechanical deformity is observed, should be recommended for physiotherapy or podiatric assessment to avert any chronic recurrence. NSAIDs and corticosteroid injections are most effective for this condition when they are combined with biomechanical correction.
Mechanical treatment that comprises taping and orthoses is known to have shown more effective results than either anti-inflammatories or accommodative modalities.
Plantar fascia night splints can be used to provide you with short-term pain relief. The night splints overstretch your plantar fascia which may give some short-term relief; however, lengthens the passive arch structures. Furthermore, the medium and long-term benefits offered by this rationale make no sense. On the other hand, permanent elongation will incline you to flatter arches and increase the chances of recurrent heel pain. Based on this assessment, we do NOT recommend the plantar fascia night splints in most cases of plantar fasciitis.
Weight loss and load management can influence the initiation & duration of plantar fasciitis and heel spur quite effectively. Your weight may be impacting your plantar fascia or heel spurs, so weight loss should be a priority for those patients who are carrying excess weight.
Researchers have concluded that there are essentially 8 stages that need to be covered to effectively rehabilitate plantar fasciitis and prevent a recurrence. These are:
Phase 1 – Early Injury Protection: Pain Relief & Anti-inflammatory Tips
The initial treatment suggested for most soft tissue injuries is Rest, Ice, and Protection. In the early phase, you are most likely unable to walk pain-free. Our primary aim is to provide some active rest to you from foot postures that provoke pain. This means that you should stop doing any movement or activity that provoked your foot pain in the first place.
Ice is a simple and effective modality that can help in reducing your pain and swelling. Please apply ice for 20-30 minutes each 2 to 4 hours during the initial phase or when you notice that your injury is warm or hot. You may also use a frozen water bottle which can serve as an ice foot roller and simultaneously provide you with some gentle plantar fascia massage.
Anti-inflammatory medication (if tolerated) and natural substances can also assist in reducing your pain and swelling. However, it is recommended to avoid any anti-inflammatory drugs during the initial 48 to 72 hours as they may lead to additional bleeding. Most people often take paracetamol as a pain reducing medication as they are able to tolerate it.
You may have to wear a plantar fascia brace, heel cups or get your foot taped to have some pain relief and support & protect your plantar fascia. As previously mentioned, the cause of your plantar fasciitis determines what type of treatment will work best for you. Your physiotherapist will guide you and provide some pain relieving techniques such as joint mobilisations for stiff joints, acupuncture, massage, electrotherapy, or dry needling to help you walk through this painful phase.
Phase 2 – Regain Full Range of Motion
If you protect your injured plantar fascia appropriately, the injured tissues will heal. When protected from additional damage, the inflamed structures settle down and help you avoid long-standing degenerative changes.
Plantar fasciitis may take several weeks (through to many months) to heal while we await Mother Nature to form and mature the new scar tissue, which takes at least six weeks. During this period, you must aim to optimally remould your scar tissue for preventing a poorly formed scar that may potentially re-tear or become lumpy in the near future. It is vital to elongate and orientate your healing scar tissue. It is done through massage, gentle stretches, and light active exercises.
In most cases, your physiotherapist will check for the presence of any stiff joints in your foot and ankle complex. If there are any stiff joints, they will be loosened to assist you to avoid plantar fascia overstress. The limited range of ankle bend during a squat manoeuvre is a sign of a stiff ankle joint. Your physiotherapist will guide you.
Phase 3 – Restore Foot Arch Muscle Control
The foot arch is controlled dynamically by the foot arch muscles, which may be either weak or have poor endurance. These foot muscles serve as the main dynamically stable base for your foot and help in preventing excessive loading through your plantar fascia.
Any deficiencies in your case can be an important part of your rehabilitation process. A physiotherapist will assess and correct your dynamic foot control. They will assist you in correcting your normal foot biomechanics and provide you with foot stabilisation exercises if required.
Phase 4 – Restore Normal Calf & Leg Muscle Control
The leg (calf, thigh and hip) muscles play a vital role in controlling the foot arch and its normal function. Your physiotherapist examines your leg muscle function and extends you the necessary treatment or exercises as per requirements.
Phase 5 – Restore Normal Foot Biomechanics
Your foot biomechanics are the main predisposing factor for plantar fasciitis. Based on your biomechanical assessment, you may have to get a soft orthotic or a custom-made orthotic prescribed by a podiatrist.
Phase 6 – Enhance Running and Landing Technique
If the cause of your plantar fasciitis is a sport, it is because of the repetitive activities which place enormous forces on your plantar fascia.
To prevent a recurrence of plantar fasciitis as you return to your sport, your physiotherapist will provide you with certain technique corrections and exercises. These techniques and exercises will help you address these important elements of rehabilitation to prevent a recurrence and enhance your performance in sports.
As per your sport or lifestyle, the physiotherapist will provide a customised program for speed, agility, proprioception and power to prepare you for light sport-specific training.
Phase 7 – Return to Sport or Work
Depending on your sport or job demands, you need to do some sport-specific or work-specific exercises. Moreover, you are also required to follow a training regime to start a safe and injury-free return to your chosen sport or employment.
After discussing your goals, time frames and training schedules with you, your physiotherapist will optimise you for a complete return to sport or work. If you face any work-related injuries, consult immediately with your doctor, rehabilitation counsellor or employer.
Phase 8 – Footwear Analysis
In most cases, it is often the poorly designed footwear that can put you at risk of an injury. For this, you need to seek professional advice from your healthcare practitioner.
Find the Perfect Insoles for Plantar Fasciitis
We at Boyner Clinic offer custom-made Insole for plantar fasciitis.
If you are struggling with plantar fasciitis, connect with us to buy the best quality insoles for plantar fasciitis today.
Experience unparalleled comfort with our specially designed plantar fasciitis high arch insoles. Our premium products offer superior support and relief, helping you walk more comfortably. Reach out to us to find the ideal insoles for your needs and take control of your foot health today. Start your journey to pain-free living now!
BoynerClinic provides targeted insoles for plantar fasciitis, perfect for high arches. These insoles are designed to relieve pain and improve comfort, contact our doctors to ensuring the best support for those with plantar fasciitis.